Radiation Oncology
Offering hope and empowerment as we team up with you in your fight against cancer.
At Valley, we provide state-of-the-art radiation therapy in a community setting, emphasizing innovative technology in a comfortable and supportive, patient-oriented environment. Our team is comprised of board certified physicians, oncology certified nursing staff, licensed radiation therapists, oncology social workers, registered dieticians, and other support staff. Our experienced specialists consult with you to develop the best care plan tailored to your specific needs, with quality of life in mind.
Your care is documented in an electronic medical record so that your entire care team has immediate access to your medical history, including procedures performed, notes and test results. Our treatment decisions are supported by NCCN (National Comprehensive Cancer Network) guidelines, which are the industry standard for cancer therapy.
Valley offers advanced radiation therapies for treatment of both cancerous and non-cancerous tumors. Our multidisciplinary radiation oncology team focuses on supporting you and your caregivers before, during and after treatment. We provide symptom management, monitor your physical and emotional well-being, educate you about treatment options and new medications, and coordinate other directed therapies.
Our focus is on YOU and providing you and your loved ones with the best treatment experience possible.
All cells grow and divide to form new cells. But cancer cells grow and divide faster than the normal cells around them and invade other tissues. Radiation therapy uses high-energy radiation to shrink tumors and kill cancer cells, thus preventing the cells from growing, dividing, and spreading.
Also referred to as radiotherapy, irradiation, or x-ray therapy, radiation therapy is one of the most common treatments for cancer. Unlike chemotherapy, which exposes the whole body to cancer-fighting drugs, radiation therapy is usually applied locally, affecting only the part of the body being treated and limiting harm to nearby healthy tissue.
What Type of Radiation Therapy is Best?
Deciding which type of radiation to use depends upon the kind of cancer you have and where it is in your body. Discuss with your radiation oncologist which type of treatment plan is right for you.
"Radiation Therapy and You" a publication by the National Cancer Institute
Types of Radiation Therapy
Radiation may be delivered by a machine outside the body (external-beam radiation therapy), or may come from radioactive material placed in the body near cancer cells (internal radiation therapy, also called brachytherapy). Radiation oncologists may also prescribe a combination of radiation therapies to treat a patient's cancer. Radiation can be given alone or used with other treatments, such as surgery or chemotherapy. In fact, certain drugs are known to be radiosensitizers. This means they can actually make the cancer cells more sensitive to radiation, which allows the radiation to better kill cancer cells.
About half of all cancer patients receive some type of radiation therapy during the course of their treatment.
External Beam Radiation Therapy
E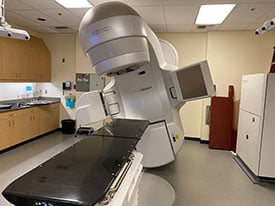 xternal radiation (or external beam radiation) uses a machine to direct high-energy x-rays from outside the body into the tumor, while minimizing radiation exposure to nearby healthy tissue. Scheduled as a series of outpatient visits, external radiation therapy is typically repeated over a period of many weeks.
xternal radiation (or external beam radiation) uses a machine to direct high-energy x-rays from outside the body into the tumor, while minimizing radiation exposure to nearby healthy tissue. Scheduled as a series of outpatient visits, external radiation therapy is typically repeated over a period of many weeks.
Watch a video:
Radiation Therapy
Valley Medical Center employs state-of-the-art treatment machines called linear accelerators that use image-guidance and x-ray technology to precisely locate tumors in real time. This is critically important since tumors can move—as a result of breathing or due to shifting caused by weight loss or other physical changes over the course of treatment. In addition, the linear accelerator is capable of mapping irregularly shaped tumors and varying the intensity and direction of beams of radiation to destroy cancerous cells and exclude healthy tissue.
There are a number of treatment plan styles available for external radiation. Selection depends upon tumor location, shape, size, proximity to organs and other factors. Discuss with your radiation oncologist which type of treatment plan is right for you.
Internal Radiation Therapy
Internal radiation (also called brachytherapy [brake-ee-THER-uh-pee]) uses a radioactive source in the form of a wire, seed, pellet, or balloon that’s called an implant. The implant is put inside the body in or near the tumor. The radiation from the implant travels only a short distance, so it has very little effect on normal body tissues. In some cases, patients may need to stay in the hospital while getting internal radiation.
Sometimes, after a tumor has been removed by surgery, radioactive implants are put into the area where the tumor was to kill any cancer cells that may still be there.
Implants may either be left in the patient as a permanent implant or they may be removed after a certain amount of time.
Brachytherapy can be given alone or in conjunction with external beam radiation therapy. Your radiation oncologist will be able to provide consultation regarding this treatment here at Valley Medical Center or refer you to appropriate specialist.
Learn more about brachytherapy in the health library.
Radiation therapy is often prescribed to treat cancer. It may be used alone or with chemotherapy, depending upon the type of cancer and location within the body.
- With external radiation therapy—also called radiotherapy— a machine called a linear accelerator (or "linac") targets a beam of radiation at the cancer site from outside the body. The radiation beam is painless and treatment itself lasts only a few minutes. Treatment is usually delivered on a daily basis (weekdays) over the course of a number of weeks.
- With internal radiation therapy—also called "brachytherapy" [brake-ee-THER-uh-pee])—a radioactive implant(s) is placed very close to or inside the tumor. The implant(s) may reside permanently inside the patient or may be removed at a later time. Treatment may require a hospital stay.
Learn more about types of radiation therapies
| |
|
Front Desk
Our friendly speciality service coordinators greet you when you check in at the radiation oncology building. During the course of your treatment here, they assist with insurance verification, appointment scheduling, medical record requests, record maintenance, and with arranging transportation for your appointments with other units within the hospital.
Nurses
Our registered nurses (RNs) have specialized education and training in the care of cancer patients undergoing radiation treatment. They also support patients' families and loved ones. Throughout your journey, the nursing staff monitors your physical and emotional well-being and helps you and your family understand your treatment plan—the type of therapy, what to expect, timelines, and how to manage potential side effects. They're available with tips to help improve your comfort level and with referrals for outside resources, as needed.
Doctors
The radiation oncologists here at Valley Medical Center are board certified physicians who specialize in radiation therapy and the treatment of cancer. The radiation oncologist oversees all aspects of the radiation treatment. This includes prescribing appropriate radiation therapy, creating a custom plan for each patient, ensuring adherence to quality-control protocols and working with you to manage your side effects. In addition, our doctors communicate with your referring physicians so that they understand your radiation plan and treatment timelines.
Find a Radiation Oncologist
What does "board certified" mean?
Radiation Therapists

Registered radiation therapists (RT) administer your daily radiation treatments using the prescription and treatment plan prescribed by the physicians, working closely with the doctors during your entire treatment course. They also perform daily quality-assurance inspection of treatment machines to ensure your treatments are administered safely and correctly.
Medical Physicist
A medical physicist makes sure equipment is calibrated and operating properly to protect the patient, care takers and medical staff from radiation exposure. Our board certified medical physicists work closely with doctors and dosimetrists in creating your custom treatment plan, including determining optimal body positioning, both for your comfort and ease of reproducibility. A physicist also checks every chart and every plan as part of our ongoing quality assurance and is responsible for the daily, monthly and yearly equipment inspections that assure we comply with state and federal regulations governing the medical administration of radiation.
Dosimetrist
In collaboration with the radiation oncologist, medical dosimetrists work closely with our medical physicists to determine the proper radiation dosage needed and optimal location of treatment on a patient's body in order to shrink or eliminate tumor growth. Our dosimetrists are board certified.
Oncology Social Worker
The oncology social worker's role is to provide psychosocial care for oncology patients, families, caregivers, and their community. Such care can encompass transportation issues, workplace issues, emotional support, education materials, family issues and securing assistance at home. The oncology social worker works primarily with outpatients and accepts referrals from multiple departments within the medical center.
Registered Dietitian
A registered dietitian promotes good health through proper diet. Our dietitian recommends a therapeutic diet to aid in the treatment of disease, and provides nutrition assessment, interventions and counseling for any individual—and their loved ones—undergoing radiation therapy.
Radiation Therapy FAQ
Radiation therapy is a curative treatment approach that strives to eliminate all cancer cells. In cases where it is not possible to completely eliminate the disease, radiation therapy can be used to shrink tumors and reduce pressure, pain, and other symptoms of cancer. This is called palliative radiation therapy, where the goal is to improve a person's quality of life.
Although you can’t see the radiation being used during your treatment, your radiation oncology team can control it using special software and radiation beam modifying devices. Doctors have been safely and effectively treating patients with radiation therapy for more than 100 years.
Radiation therapy slightly increases the risk of developing a second cancer. However, it is important to remember that in many cases, radiation therapy can eliminate the current, existing cancer. This benefit far outweighs the small risk that the treatment could cause a new cancer later in life.
The effect on the surrounding areas of the body depends on the type and location of the radiation. For example, men with prostate cancer who receive radiation therapy to the prostate may experience bowel or bladder problems because these organs are located very close to each other. As much as possible, the radiation is aimed precisely at the tumor to avoid harming surrounding organs. Talk with your doctor to learn what parts of your body could be affected by radiation therapy and how to manage common side effects of treatment.
Radiation from the machine cannot be seen, felt or smelled; so there is no need to worry that a treatment session will be painful.
For some people, radiation therapy causes few or no side effects. For others, the side effects are more severe. No two cancers and no two patients are exactly alike; therefore, each radiation treatment is individually customized by your radiation oncologist. If a side effect develops, it is often during the latter part of your treatment course. Many side effects begin to resolve a few weeks after the final radiation treatment. Your radiation treatment team will work with you to ease or prevent many of these side effects.
Radiation therapy to the pelvic area can affect the reproductive system. For some women, permanent infertility (the inability to conceive a child or maintain a pregnancy) can occur, but usually only if both ovaries receive radiation. Men receiving radiation therapy to the testes or to nearby organs, such as the prostate, will have lowered sperm counts and reduced sperm activity, which affects fertility (the ability to father a child). If you are worried your treatment plan may reduce your fertility, talk to your healthcare team before treatment begins. There are a number of ways to preserve your fertility.
Radiation therapy is a local treatment, meaning it only affects the area of the body where the tumor is located. People do not lose their hair from having radiation therapy unless it is aimed at a part of the body that grows hair, such as the scalp.
External-beam radiation therapy does not make a person radioactive at any time. The radiation is delivered to the body from a machine located in the treatment room so there is no radiation left behind once the treatment machine is turned off. However, with internal radiation therapy (also called low dose brachytherapy), the implants placed in the patient's body deliver most of the radiation to the cancer, but some radiation can be emitted (released). Therefore, people who receive internal radiation therapy need to take specific precautions for a period of time outlined by your doctor to reduce others’ exposure to the radiation.
Some types of cancer respond best to combination treatment approaches that may include radiation plus surgery, chemotherapy, or immunotherapy. For other types of cancer, radiation therapy alone is often an effective treatment.